Custom Implant Materials
The choice of materials for medical implants is a critical decision that significantly impacts patient outcomes. In the realm of aesthetic and reconstructive surgery, the material not only needs to fulfill functional requirements but also must align with the patient’s body response and long-term health. The medical device industry plays a pivotal role in this decision-making process, often influencing the choices of surgeons through partnerships, commissions, and educational incentives. Such influence can sometimes lead to a preference for certain materials over others, potentially based not solely on clinical efficacy but also on business relationships.
This blog post delves into the various materials used in medical implants, focusing on their advantages, limitations, and the ethical considerations surrounding their use. We will explore how different materials affect the surgical outcome, healing time, and the risk of complications such as infections. Furthermore, the post will analyze how market forces and regulatory frameworks influence material choices, ensuring that surgeons and patients are well-informed to make the best decisions for health and functionality.
Key Questions for Surgeons
When choosing implants, surgeons consider several factors:
- Surgical Adjustments: How much intraoperative modification is acceptable?
- Risk Assessment: What level of infection risk is manageable?
- Material Selection: Which materials are prone to complications like pocket formations?
Key Questions for Patients
Do you believe that a single procedure could meet all your expectations for the rest of your life? While we hope for the best, it is prudent to prepare for the possibility of future adjustments. Most patients find that their needs or conditions change over time, which may necessitate additional procedures.

To ensure you are prepared, it’s essential to discuss with your surgeon the long-term considerations of different implant materials. Specifically, ask which materials are associated with the easiest replacement processes and the lowest risk of infection. This information will help you make a more informed decision about your care.
Material Comparisons for Facial Implants
Ease of Malleability
- Highly Malleable: Silicone and silicone rubber, are known for excellent malleability, making them an easy material to fiddle with during surgery.
- Moderately Malleable: Materials like porous polyethylene offer good malleability but are not as easy to manipulate as silicone.
- Less Malleable: Titanium and PEEK are less flexible and often come in pre-shaped forms, which may require specialized tools for adjustments during surgery.
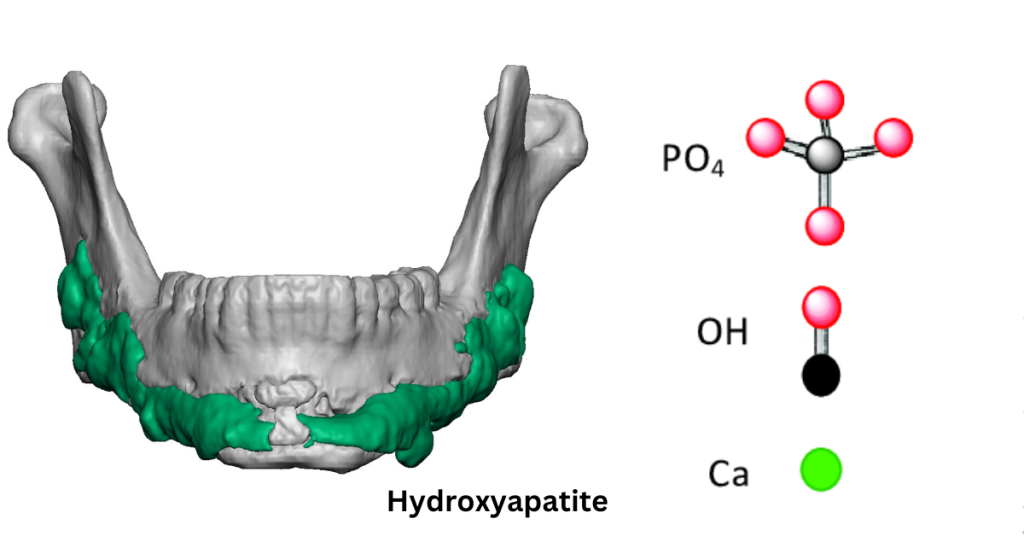
- Paste or Powder Form Implants: Implants such as PMMA (bone cement) and hydroxyapatite can be molded during surgery or injected in paste form. However, it’s important to note that once these materials are set, removing them can be highly challenging. Patients should consider this factor when discussing implant options with their surgeon, as it affects the feasibility of future modifications or removal.
Implantation Time and Potential Drawbacks During Surgery
- Malleable Materials: Typically allow for quicker implantation times because they can be easily adjusted to fit the surgical site.
- Rigid Materials: This may require longer surgery times due to the need for precise pre-surgical planning and possibly intraoperative modifications.
Accessibility and Cost
- Common Materials (e.g., Silicone, Polyethylene): Generally more accessible and less expensive, making them popular choices for a wide range of medical facilities.
- Specialized Materials (e.g., PEEK, Titanium): Can be more expensive and might require special ordering processes, impacting their availability.
Staff Training
- Malleable Materials: Generally require basic surgical training as these materials are easier to handle and shape.
- Advanced Materials (e.g., Titanium, PEEK): This may require additional training for the medical staff due to their specific handling and shaping requirements during implantation.
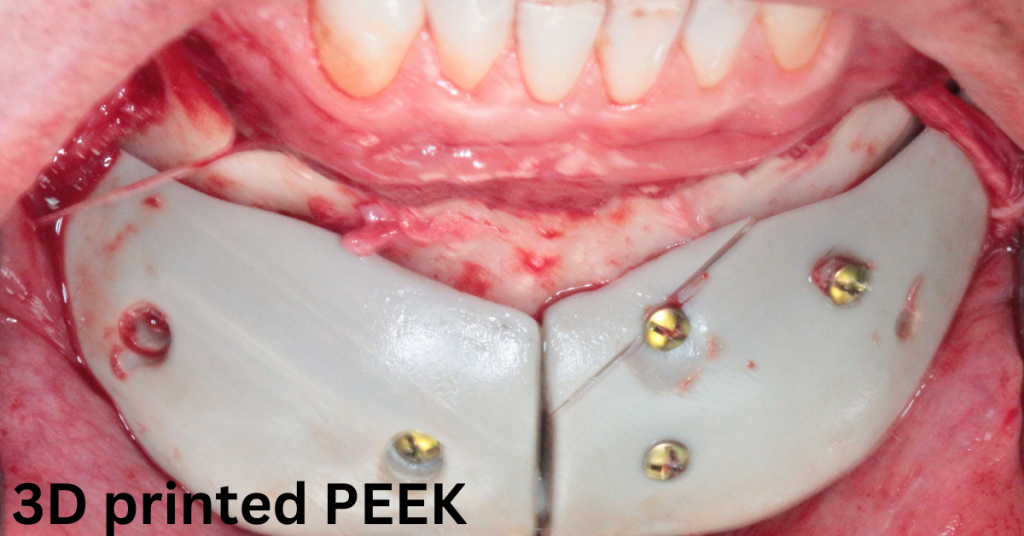
Shifting Focus to Synthetic Materials: Analyzing PEEK
Original Purpose and Adoption
While synthetic materials are increasingly popular in medical implants due to their versatile properties, Polyether ether ketone (PEEK) serves as a prime example of this shift.
Polyether ether ketone (PEEK) was initially developed to replace metals in engineering applications requiring weight reduction without sacrificing strength, stiffness, or resistance to heat and chemicals. It found uses in aerospace, automotive, and chemical processing industries. Due to its properties, PEEK has become an attractive option in the medical implant field, favored for its biocompatibility and durability.
Manufacturing Advantages
PEEK’s adaptability for 3D printing has made it a popular choice in the medical implant industry. This manufacturing method offers ease and convenience but requires careful assessment to ensure PEEK is the right choice for aesthetic implants.
Regulatory and Ethical Considerations
- Regulations: Surgeons are generally aware of the risks associated with different materials and the regulatory environments, which can vary significantly by country.
- Ethical Concerns: There is a potential conflict of interest when surgeons have a financial stake in the implants they use, which could influence their choice, potentially prioritizing personal gain over patient welfare.
Infection Rates and Tissue Integration
The relationship between the integration of implant materials with surrounding tissues and reduced infection rates hinges on several factors:
- Improved Tissue Adherence: When materials are capable of integrating well with surrounding tissues, they form a more cohesive interface. This tight integration means fewer gaps between the implant and the tissue, minimizing spaces where bacteria can thrive and potentially reducing the risk of infection.
- Reduced Foreign Body Response: Materials that integrate well with tissues are less likely to provoke a significant foreign body reaction. A pronounced foreign body response can lead to inflammation, compromising the tissue’s natural defenses against infection.
- Stability of the Implant: Well-integrated materials tend to be more stable within their implant site. Stability is crucial because the movement of the implant can cause micro-tears or damage to surrounding tissues, which can serve as entry points for bacteria and lead to infection.
- Enhanced Healing: When implants integrate well, they often support not just mechanical stability but also promote cellular growth and tissue healing around the implant. Faster and more effective healing can help seal off potential entry points for infection more quickly.
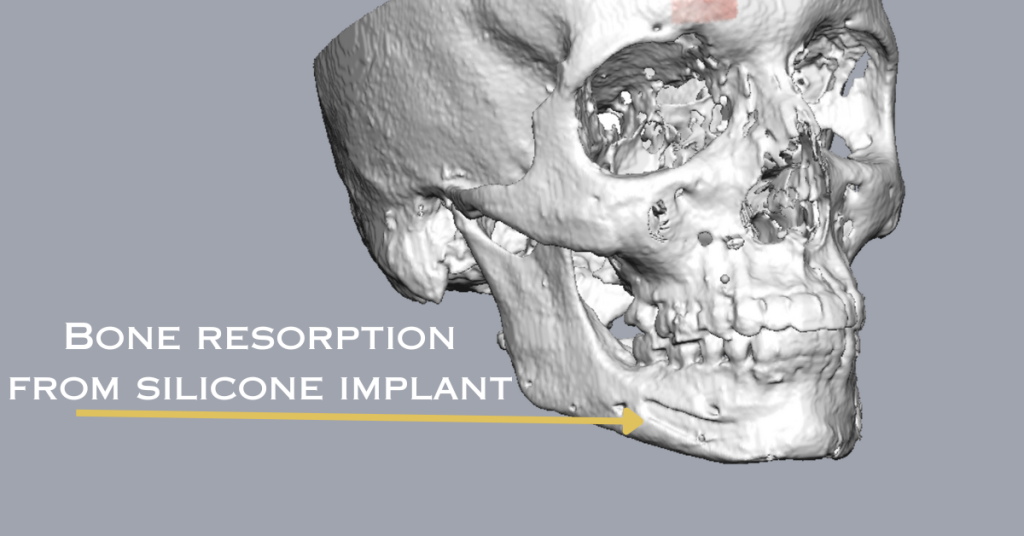
Understanding Bone Erosion and Resorption with Implant Materials
Bone erosion presents a significant challenge when using implant materials. This condition occurs when the implant material interacts negatively with the surrounding bone, irrespective of the material’s hardness or the implantation method (such as screwing or suturing). Bone erosion results from a combination of mechanical stress and biological reactions, which undermines the stability and integrity of the surrounding bone. As the bone adjacent to the implant degrades over time, understanding this dynamic is vital for selecting the right implant materials, as it greatly affects the implant’s durability and effectiveness.
Key Differences Between Bone Erosion and Bone Resorption
- Mechanism:
- Bone Erosion: Directly caused by adverse interactions between the implant material and the bone, often exacerbated by mechanical stress and biological responses.
- Bone Resorption: A natural physiological process where osteoclasts break down bone tissue, which can be accelerated by pressure from the implant.
- Impact on Implant Success:
- Bone Erosion: Leads to the degradation of bone around the implant, threatening the implant’s stability and requiring careful material selection.
- Bone Resorption: Although it can compromise implant stability if excessive, it is a normal aspect of bone turnover and can be managed with careful implant design and placement.
Understanding these distinctions helps in the strategic planning and management of implants to optimize their longevity and functionality.

DMI Implants: A Case Study in Innovation and Integration
DMI implants represent a significant advancement in implant technology, especially in terms of material innovation and application. These implants are moderately malleable, allowing for easier intraoperative modifications compared to rigid materials like PEEK or titanium. Unlike silicone or Goretex, DMI implants can be cut more readily during surgery, providing a practical balance between flexibility and stability.
Key features of DMI implants include:
- Material Composition: DMI implants promote osseointegration—the process by which an implant integrates with existing bone tissue. Has the capability to promote tissue ingrowth, though not as extensively as Goretex, since it doesn’t completely penetrate the material.
- Surgical Adaptability: The malleability of DMI implants allows surgeons to make precise cuts and adjustments during implantation, which is less feasible with materials like PEEK or titanium.
- Biocompatibility and Integration: The DMI implants facilitate bone bonding but also mimic the natural functionality of bone, reducing the risk of infection and promoting faster healing.
Comparative Analysis of Implant Materials
- Silicone and Silicone Rubber: Highly malleable, and easy to manipulate during surgery.
- Porous Polyethylene (Goretex): Offers good malleability and excellent tissue integration but can be difficult to remove once integrated.
- Titanium and PEEK: Less flexible, often requiring specialized tools for adjustments.
- PMMA and Hydroxyapatite: These can be molded or injected during surgery but are challenging to remove once set.
Conclusion: The Need for Informed Choices and Further Dialogue
Choosing the right material for implants is a complex decision that should prioritize patient safety and long-term health outcomes. Continued dialogue among practitioners and patients is crucial to achieving the best possible results in the field of aesthetic implants.
The Importance of the Surgeon’s Experience
An experienced surgeon, familiar with various materials and their specific requirements, will likely achieve better outcomes. Each patient presents unique challenges, and a well-equipped surgeon can effectively address these with their chosen material and techniques.